
Discrimination at work is linked to high blood pressure

Experiencing discrimination in the workplace — where many adults spend one-third of their time, on average — may be harmful to your heart health.
A 2023 study in the Journal of the American Heart Association found that people who reported high levels of discrimination on the job were more likely to develop high blood pressure than those who reported low levels of workplace discrimination.
Workplace discrimination refers to unfair conditions or unpleasant treatment because of personal characteristics — particularly race, sex, or age.
How can discrimination affect our health?
“The daily hassles and indignities people experience from discrimination are a specific type of stress that is not always included in traditional measures of stress and adversity,” says sociologist David R. Williams, professor of public health at the Harvard T.H. Chan School of Public Health.
Yet multiple studies have documented that experiencing discrimination increases risk for developing a broad range of factors linked to heart disease. Along with high blood pressure, this can also include chronic low-grade inflammation, obesity, and type 2 diabetes.
More than 25 years ago, Williams created the Everyday Discrimination Scale. This is the most widely used measure of discrimination’s effects on health.
Who participated in the study of workplace discrimination?
The study followed a nationwide sample of 1,246 adults across a broad range of occupations and education levels, with roughly equal numbers of men and women.
Most were middle-aged, white, and married. They were mostly nonsmokers, drank low to moderate amounts of alcohol, and did moderate to high levels of exercise. None had high blood pressure at the baseline measurements.
How was discrimination measured and what did the study find?
The study is the first to show that discrimination in the workplace can raise blood pressure.
To measure discrimination levels, researchers used a test that included these six questions:
- How often do you think you are unfairly given tasks that no one else wanted to do?
- How often are you watched more closely than other workers?
- How often does your supervisor or boss use ethnic, racial, or sexual slurs or jokes?
- How often do your coworkers use ethnic, racial, or sexual slurs or jokes?
- How often do you feel that you are ignored or not taken seriously by your boss?
- How often has a coworker with less experience and qualifications gotten promoted before you?
Based on the responses, researchers calculated discrimination scores and divided participants into groups with low, intermediate, and high scores.
- After a follow-up of roughly eight years, about 26% of all participants reported developing high blood pressure.
- Compared to people who scored low on workplace discrimination at the start of the study, those with intermediate or high scores were 22% and 54% more likely, respectively, to report high blood pressure during the follow-up.
How could discrimination affect blood pressure?
Discrimination can cause emotional stress, which activates the body’s fight-or-flight response. The resulting surge of hormones makes the heart beat faster and blood vessels narrow, which causes blood pressure to rise temporarily. But if the stress response is triggered repeatedly, blood pressure may remain consistently high.
Discrimination may arise from unfair treatment based on a range of factors, including race, gender, religious affiliation, or sexual orientation. The specific attribution doesn’t seem to matter, says Williams. “Broadly speaking, the effects of discrimination on health are similar, regardless of the attribution,” he says, noting that the Everyday Discrimination Scale was specifically designed to capture a range of different forms of discrimination.
What are the limitations of this study?
One limitation of this recent study is that only 6% of the participants were nonwhite, and these individuals were less likely to take part in the follow-up session of the study. As a result, the study may not have fully or accurately captured workplace discrimination among people from different racial groups. In addition, blood pressure was self-reported, which may be less reliable than measurements directly documented by medical professionals.
What may limit the health impact of workplace discrimination?
At the organizational level, no studies have directly addressed this issue. Preliminary evidence suggests that improving working conditions, such as decreasing job demands and increasing job control, may help lower blood pressure, according to the study authors. In addition, the American Heart Association recently released a report, Driving Health Equity in the Workplace, that aims to address drivers of health inequities in the workplace.
Encouraging greater awareness of implicit bias may be one way to help reduce discrimination in the workplace. Implicit bias refers to the unconscious assumptions and prejudgments people have about groups of people that may underlie some discriminatory behaviors. You can explore implicit biases with these tests, which were developed at Harvard and other universities.
On an individual level, stress management training can reduce blood pressure. A range of stress-relieving strategies may offer similar benefits. Regularly practicing relaxation techniques or brief mindfulness reflections, learning ways to cope with negative thoughts, and getting sufficient exercise can help.
About the Author

Julie Corliss, Executive Editor, Harvard Heart Letter
Julie Corliss is the executive editor of the Harvard Heart Letter. Before working at Harvard, she was a medical writer and editor at HealthNews, a consumer newsletter affiliated with The New England Journal of Medicine. She … See Full Bio View all posts by Julie Corliss
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

How well do you score on brain health?

Need another jolt of motivation to shore up a resolution to shed weight, sleep more soundly, boost nutrition or exercise levels, or cut back on alcohol? Then you'll be pleased to learn that any (and all) of these efforts can also add up to better brain health.
An international study led by researchers at the McCance Center for Brain Health at Massachusetts General Hospital devised and validated a Brain Care Score (BCS) card that makes it easy to total up what you're doing well and where you might do better. The prize is a healthier brain — specifically a lower risk for dementia and strokes.
Designed to predict how current habits might impact future brain health, the user-friendly scorecard is apparently the first of its kind, says Dr. Andrew Budson, a lecturer in neurology at Harvard Medical School.
"It's a real service that the researchers have developed a scale like this and completed the first study to determine if scoring worse on this scale raises your risk for dementia and stroke," says Dr. Budson, who wasn't involved in the analysis. "On one hand, no one's done something quite like this before. On the other, however, it's really wrapping together health factors everyone has known for a number of years in new packaging."
What's included on the scorecard?
Called the McCance Brain Care Score, the card tallies points from 12 physical, lifestyle, and social-emotional domains.
Physical components relate to
- blood pressure
- blood sugar
- cholesterol
- body mass index (BMI).
Lifestyle components include
- nutrition
- alcohol intake
- smoking
- aerobic activities
- sleep.
Social-emotional factors inquire about
- stress management
- social relationships
- meaning in life.
Each response is given a score of 0, 1, or 2, with the highest possible score totaling 21. Higher scores suggest better brain care.
"All these physical and lifestyle factors can contribute to the risk of dementia to some extent through strokes," Dr. Budson says. "Those that aren't a risk through strokes are usually related to the fact that a healthy brain is a brain that's using all of its parts. Engaging in healthy relationships and meaningful activities helps us maintain good brain structure and function."
What did the analysis involve?
The study was published online in Frontiers of Neurology in December 2023. It involved nearly 399,000 adults ages 40 through 69 (average age 57; 54% women) who contributed personal health information to the UK Biobank.
During an average follow-up period of 12.5 years, participants recorded 5,354 new cases of dementia and 7,259 strokes. Researchers found that participants with higher Brain Care Scores at the study's start had lower risks of developing dementia or strokes over time.
These threats to health and independence take a stunning — and growing — toll on people in the US. Dementia affects one in seven Americans, a rate expected to triple by 2050. Meanwhile, more than 795,000 people in the United States suffer a stroke each year, according to the CDC.
What did the study find?
Each five-point step higher in the BCS rating assigned when the study began was linked to significantly lower risks of dementia and stroke, with those odds varying by age group:
- Participants younger than 50 at the study's start were 59% less likely to develop dementia and 48% less likely to have a stroke with each five-point higher score on BCS.
- Participants 50 through 59 at the study's start were 32% less likely to develop dementia and 52% less likely to have a stroke with each five-point higher score on BCS.
But those brain disease benefits appeared to diminish for those older than 59 at the study's start. This group experienced only 8% lower odds of dementia and a 33% lower risk of stroke with each five-point higher score on BCS. Study authors theorized that some of these participants may have already been experiencing early dementia, which is difficult to detect until it progresses.
"I feel very comfortable that the study's conclusions are entirely correct, because all the factors that go into its BCS are well-known things people can do to reduce their risk of stroke and dementia," Dr. Budson says.
What are the study's limitations?
However, Dr. Budson notes that the study did have a couple of limitations,. The UK Biobank fell just short of collecting all the components of the BCS in its dataset, lacking meaning-of-life questions. So its scores ranged from 0 to 19, not up to 21. "It's a practical limitation, but it should be acknowledged that so far, there have been no studies to validate the actual 21-point scale they're recommending we use," he says.
The analysis also evaluated participants' scores at just one point in time instead of several, Dr. Budson says. Future research should determine whether people can lower their stroke and dementia risk by improving their BCS over time with behavior and lifestyle changes.
How can you play this game at home?
While better brain health may be the clear prize of a higher score, it's far from the only benefit. That's because improving any health component of the BCS also benefits our overall well-being.
"By improving these factors, not only will people help their brain, but they'll also help their heart and reduce their risk of cancer," Dr. Budson adds. "These factors will absolutely also improve your psychological health, which is certainly an important part of brain health."
The scale's simple breakdown of health factors also makes it easy to focus on tweaking one or two without getting overwhelmed.
"Let's say someone's nutrition isn't perfect — and they know it — but they're not willing to change their diet. Fine. They can then decide to do more aerobic exercise, for example, or to stop drinking, or to get the sleep their body needs," he says.
What one change could put you on a path to better brain health?
If he had to choose just one factor to improve brain health, Dr. Budson would focus on meaning of life, "which means you generally feel your life has meaning or purpose," he says. To do that, he suggests giving deep, quiet thought to what you wish your life's purpose to be, whether you expect to live a long time or just a few years.
"Once you have a purpose, then you have a reason to follow through with assessing all the other items on the BCS scale and seeing what you can do so you'll be around longer, and be competent and capable longer, to help fulfill the meaning and purpose of your life," he says.
About the Author

Maureen Salamon, Executive Editor, Harvard Women's Health Watch
Maureen Salamon is executive editor of Harvard Women’s Health Watch. She began her career as a newspaper reporter and later covered health and medicine for a wide variety of websites, magazines, and hospitals. Her work has … See Full Bio View all posts by Maureen Salamon
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Do children get migraine headaches? What parents need to know

Headaches are very common in children and teens. In fact, more than half will suffer from headaches at some point, and by 18 years the majority of adolescents have had them. And while most headaches are part of a viral illness, some are migraines. In fact, recurring migraines affect as many as one in 10 children and teens overall.
What should you know — and do — if you think your child or teen may be having migraines?
How early do migraines start to occur?
We don’t tend to think about migraines in children, but by age 10, one in 20 children has had a migraine. And migraines sometimes occur even earlier.
Before puberty, boys and girls are equally likely to have them. After puberty, migraines are more common in girls.
Which migraine symptoms are most common in children?
Migraines are often one-sided in adults. In children they are more likely to be felt on both sides of the head, either in both temples or both sides of the forehead.
While it’s not always easy to tell a migraine from another kind of headache, children
- often report throbbing pain
- may experience nausea and sensitivity to light and noise.
The flashing lights and other vision changes people often see as a migraine begins are less common in children. However, parents may notice that their child is more tired, irritable, or pale before a migraine begins — and takes a while to get back to normal after it ends.
What causes migraines in children?
We don’t know exactly what causes migraines. We used to think it had to do with blood flow to the brain, but that does not seem to be the case. It appears that migraines are caused by the nerves being more sensitive, and more reactive to stimulation. That stimulation could be stress, fatigue, hunger, almost anything.
Migraines run in families. In fact, most migraine sufferers have someone in the family who gets migraines too.
Can migraines be prevented?
The best way to prevent migraines is to identify and avoid triggers. The triggers are different in each person, which is why it’s a good idea to keep a headache diary.
When your child gets a headache, write down what was happening before the headache, how badly it hurt and where, what helped, and anything else about it you can think of. This helps you and your doctor see patterns that can help you understand your child’s particular triggers.
It’s a good idea to make sure your child gets enough sleep, eats regularly and healthfully, drinks water regularly, gets exercise, and manages stress. Doing this not only helps prevent migraines, but is also good for overall health!
How can you help your child ease a migraine?
When a migraine strikes, sometimes just lying down in a dark, quiet room with a cool cloth on the forehead is enough. If it’s not, ibuprofen or acetaminophen can be helpful; your doctor can tell you the best dose for your child.
It’s important not to give your child these medications more than about 14 days a month, as giving them more often can lead to rebound headaches and make everything worse!
Are there prescription medicines that can help children with migraines?
If those approaches aren’t enough, a class of medications called triptans can be helpful in stopping migraines in children ages 6 and up.
If a child experiences frequent or severe migraines, leading to missed days of school or otherwise interfering with life, doctors often use medications to prevent migraines. There are a number of different kinds, and your doctor can advise you on what would be best for your child.
Some girls get migraines around the time of their period. If that happens frequently, sometimes taking a prevention medicine around the time of menses each month can be helpful.
When to contact your doctor
If you think your child might be having migraines, you should call and make an appointment. Bring the headache diary with you. Your doctor will ask a bunch of questions, do a physical examination, and make a diagnosis. Together you can come up with the best plan for your child.
You should always call your doctor, or go to an emergency room, if your child has a severe headache, a stiff neck, trouble with coordination or movement, is abnormally sleepy, or isn’t talking or behaving normally.
The American Academy of Pediatrics has additional useful information about migraines, and how to treat and prevent them, on their website.
About the Author

Claire McCarthy, MD, Senior Faculty Editor, Harvard Health Publishing
Claire McCarthy, MD, is a primary care pediatrician at Boston Children’s Hospital, and an assistant professor of pediatrics at Harvard Medical School. In addition to being a senior faculty editor for Harvard Health Publishing, Dr. McCarthy … See Full Bio View all posts by Claire McCarthy, MD
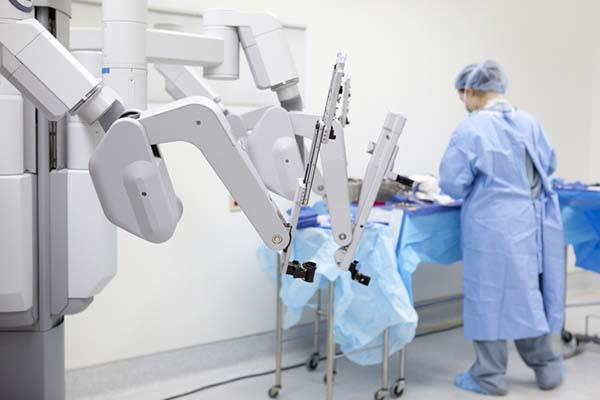
What complications can occur after prostate cancer surgery?

Earlier this year, US defense secretary Lloyd Austin was hospitalized for complications resulting from prostate cancer surgery. Details of his procedure, which was performed on December 22, were not fully disclosed. Press statements from the Pentagon indicated that Austin had undergone a minimally invasive prostatectomy, which is an operation to remove the prostate gland. Minimally invasive procedures are performed using robotic instruments passed through small “keyhole” incisions in the patient’s abdomen.
Just over a week later, Austin developed severe abdominal, hip, and leg pain. He was admitted to the intensive care unit at Walter Reed Hospital on January 2 for monitoring and further treatment. Doctors discovered that Austin had a urinary tract infection and fluid pooling in his abdomen that were impairing bowel functioning. The defense secretary was successfully treated, but then readmitted to the ICU on February 11 for what the Pentagon described as “an emergent bladder issue.” Two days after undergoing what was only described as a “non-surgical procedure performed under general anesthesia,” Austin was back at work. His cancer prognosis is said to be excellent.
Austin’s ordeal was covered extensively in the media. Although we cannot speculate about his specific case, to help our readers better understand the complications that might occur after a prostatectomy, I spoke with Dr. Boris Gershman, a urologist at Harvard-affiliated Beth Israel Deaconess Medical Center in Boston. Dr. Gershman is also a member of the advisory and editorial board for the Harvard Medical School Guide to Prostate Diseases.
How common are urinary tract infections after a prostatectomy?
Minimally invasive prostatectomy is generally well tolerated. In one study that examined complications among over 29,000 men who had the operation, the rate of urinary tract infections was only 2.1%. The risk of sepsis — a more serious condition that occurs if the body’s response to an infection damages other organs — is much lower than that.
How would a urinary tract infection occur?
Although urinary tract infections are rare after prostatectomy, bacteria can travel into the urinary system through a catheter. An important part of a prostatectomy involves connecting the urethra — which is a tube that carries urine out of the body — directly to the bladder after the prostate has been taken out. As a last step in that process, we pass a catheter [a soft silicone tube] through the urethra and into the bladder to promote healing. Infection risks are minimized by giving antibiotics both during surgery and then again just prior to removing the catheter one to two weeks after the operation.
How do you treat urinary infectious complications when they do happen?
It’s not unusual to find small amounts of bacteria in the urine whenever you use a catheter. Normally they don’t cause any symptoms, but if infectious complications do occur, then we’ll admit the patient to the hospital and treat with broad-spectrum antibiotics that treat many different kinds of bacteria at once. We’ll also obtain a urine culture to identify the bacterial species causing the infection. Based on culture results, we can switch to different antibiotics that attack those microbes specifically. The course of treatment generally lasts 10 to 14 days.
Lloyd Austin also had gastrointestinal complications. Why might that have occurred?
Although I cannot speculate about Austin’s specific case, in general gastrointestinal complications are very rare — affecting fewer than 2% of patients treated using robotic methods. However, a few different things can happen. For instance, the small intestine can “fall asleep” after surgery, meaning it temporarily stops moving food and wastes through the bowel.
This is called an ileus. It can be due to multiple reasons, including as a result of anesthetics or pain medications. An ileus generally resolves on its own if patients avoid food or water by mouth for several days. If it causes too much pressure in the bowel, then we “decompress” the stomach by removing accumulated fluids through a nasogastric tube, which is threaded into the stomach through the nose and throat.
Some patients develop a different sort of surgical complication called a small bowel obstruction. We treat these the same way: by withholding food and water by mouth and removing fluids with a nasogastric tube if necessary. If the blockages are caused by scar tissues, in rare cases this may require a second surgery to fix the obstructing scar tissue.
Fluids might also collect in the pelvis after lymph nodes are removed during surgery. What’s happening in these cases?
Pelvic lymph nodes that drain the prostate are commonly removed during prostatectomy to determine if there is any cancer spread to the lymph nodes. A possible risk from lymph node removal is that lymph fluid might leak out after the procedure and pool up in the pelvis. This is called a lymphocele. Most lymphoceles are asymptomatic, but infrequently they may become infected. When that happens, we treat with antibiotics, and we might drain the lymphocele using a percutaneous catheter [which is placed through the skin]. Fortunately, newer surgical techniques are helping to ensure that lymphoceles occur very rarely.
Are there individual factors that increase the risk of prostatectomy complications?
Certainly, patients can have risk factors for infection. Diabetes, for instance, can inhibit the immune system, especially when patients have poor glycemic or glucose control [a limited ability to maintain normal blood sugar levels]. If patients have autoimmune diseases, or if they’re taking immunosuppressive medications, they may also be at increased risk of infectious or wound healing complications with surgery, and in some cases, may instead be treated with radiation to avoid these risks.
Thanks for walking me through this complex topic! Any parting thoughts for our readers?
It’s important to discuss the potential risks of surgery with your doctor so you can be fully informed. That said, prostatectomy these days using the minimally invasive approach has a very favorable risk profile. The majority of patients do really well, and fortunately severe complications requiring hospital readmission are very rare.
About the Author

Charlie Schmidt, Editor, Harvard Medical School Annual Report on Prostate Diseases
Charlie Schmidt is an award-winning freelance science writer based in Portland, Maine. In addition to writing for Harvard Health Publishing, Charlie has written for Science magazine, the Journal of the National Cancer Institute, Environmental Health Perspectives, … See Full Bio View all posts by Charlie Schmidt
About the Reviewer

Marc B. Garnick, MD, Editor in Chief, Harvard Medical School Annual Report on Prostate Diseases; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Marc B. Garnick is an internationally renowned expert in medical oncology and urologic cancer. A clinical professor of medicine at Harvard Medical School, he also maintains an active clinical practice at Beth Israel Deaconess Medical … See Full Bio View all posts by Marc B. Garnick, MD

What is a tongue-tie? What parents need to know

The tongue is secured to the front of the mouth partly by a band of tissue called the lingual frenulum. If the frenulum is short, it can restrict the movement of the tongue. This is commonly called a tongue-tie.
Children with a tongue-tie can’t stick their tongue out past their lower lip, or touch their tongue to the top of their upper teeth when their mouth is open. When they stick out their tongue, it looks notched or heart-shaped. Since babies don’t routinely stick out their tongues, a baby’s tongue may be tied if you can’t get a finger underneath the tongue.
How common are tongue-ties?
Tongue-ties are common. It’s hard to say exactly how common, as people define this condition differently. About 8% of babies under age one may have at least a mild tongue-tie.
Is it a problem if the tongue is tied?
This is really important: tongue-ties are not necessarily a problem. Many babies, children, and adults have tongue-ties that cause them no difficulties whatsoever.
There are two main ways that tongue-ties can cause problems:
- They can cause problems with breastfeeding by making it hard for some babies to latch on well to the mother’s nipple. This causes difficulty with feeding for the baby and sore nipples for the mother. It doesn’t happen to all babies with a tongue-tie; many of them can breastfeed successfully. Tongue-ties are not to blame for gassiness or fussiness in a breastfed baby who is gaining weight well. Babies with tongue-ties do not have problems with bottle-feeding.
- They can cause problems with speech. Some children with tongue-ties may have difficulty pronouncing certain sounds, such as t, d, z, s, th, n, and l. Tongue-ties do not cause speech delay.
What should you do if think your baby or child has a tongue-tie?
If you think that your newborn is not latching well because of a tongue-tie, talk to your doctor. There are many, many reasons why a baby might not latch onto the breast well. Your doctor should take a careful history of what has been going on, and do a careful examination of your baby to better understand the situation.
You should also have a visit with a lactation specialist to get help with breastfeeding — both because there are lots of reasons why babies have trouble with latching on, and also because many babies with a tongue-tie can nurse successfully with the right techniques and support.
Talk to your doctor if you think that a tongue-tie could be causing problems with how your child pronounces words. Many children just take some time to learn to pronounce certain sounds. It is also a good idea to have an evaluation by a speech therapist before concluding that a tongue-tie is the problem.
What can be done about a tongue-tie?
When necessary, a doctor can release a tongue-tie using a procedure called a frenotomy. A frenotomy can be done by simply snipping the frenulum, or it can be done with a laser.
However, nothing should be done about a tongue-tie that isn’t causing problems. While a frenotomy is a relatively minor procedure, complications such as bleeding, infection, or feeding difficulty sometimes occur. So it’s never a good idea to do it just to prevent problems in the future. The procedure should only be considered if the tongue-tie is clearly causing trouble.
It’s also important to know that clipping a tongue-tie doesn’t always solve the problem, especially with breastfeeding. Studies do not show a clear benefit for all babies or mothers. That’s why it’s important to work with a lactation expert before even considering a frenotomy.
If a newborn with a tongue-tie isn’t latching well despite strong support from a lactation expert, then a frenotomy should be considered, especially if the baby is not gaining weight. If it is done, it should be done early on and by someone with training and experience in the procedure.
What else should parents know about tongue-tie procedures?
Despite the fact that the evidence for the benefits of frenotomy is murky, many providers are quick to recommend them. If one is being recommended for your child, ask questions:
- Make sure you know exactly why it is being recommended.
- Ask whether there are any other options, including waiting.
- Talk to other health care providers on your child’s care team, or get a second opinion.
About the Author

Claire McCarthy, MD, Senior Faculty Editor, Harvard Health Publishing
Claire McCarthy, MD, is a primary care pediatrician at Boston Children’s Hospital, and an assistant professor of pediatrics at Harvard Medical School. In addition to being a senior faculty editor for Harvard Health Publishing, Dr. McCarthy … See Full Bio View all posts by Claire McCarthy, MD

Is chronic fatigue syndrome all in your brain?

Chronic fatigue syndrome (CFS) –– or myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), to be specific –– is an illness defined by a group of symptoms. Yet medical science always seeks objective measures that go beyond the symptoms people report.
A new study from the National Institutes of Health (NIH) has performed more diverse and extensive biological measurements of people experiencing CFS than any previous research. Using immune testing, brain scans, and other tools, the researchers looked for abnormalities that might drive health complaints like crushing fatigue and brain fog. Let’s dig into what they found and what it means.
What was already known about chronic fatigue syndrome?
In people with chronic fatigue syndrome, there are underlying abnormalities in many parts of the body: The brain. The immune system. The way the body generates energy. Blood vessels. Even in the microbiome, the bacteria that live in the gut. These abnormalities have been reported in thousands of published studies over the past 40 years.
Who participated in the NIH study?
Published in February in Nature Communications, this small NIH study compared people who developed chronic fatigue syndrome after having some kind of infection with a healthy control group.
Those with CFS had been perfectly healthy before coming down with what seemed like just a simple “flu”: sore throat, coughing, aching muscles, and poor energy. However, unlike their experiences with past flulike illnesses, they did not recover. For years, they were left with debilitating fatigue, difficulty thinking, a flare-up of symptoms after exerting themselves physically or mentally, and other symptoms. Some were so debilitated that they were bedridden or homebound.
All the participants spent a week at the NIH, located outside of Washington, DC. Each day they received different tests. The extensive testing is the great strength of this latest study.
What are three important findings from the study?
The study had three key findings, including one important new discovery.
First, as was true in many previous studies, the NIH team found evidence of chronic activation of the immune system. It seemed as if the immune system was engaged in a long war against a foreign microbe — a war it could not completely win and therefore had to keep fighting.
Second, the study found that a part of the brain known to be important in perceiving fatigue and encouraging effort — the right temporal-parietal area — was not functioning normally. Normally, when healthy people are asked to exert themselves physically or mentally, that area of the brain lights up during an MRI. However, in the people with CFS it lit up only dimly when they were asked to exert themselves.
While earlier research had identified many other brain abnormalities, this one was new. And this particular change makes it more difficult for people with CFS to exert themselves physically or mentally, the team concluded. It makes any effort like trying to swim against a current.
Third, in the spinal fluid, levels of various brain chemicals called neurotransmitters and markers of inflammation differed in people with CFS compared with the healthy comparison group. The spinal fluid surrounds the brain and reflects the chemistry of the brain.
What else did study show?
There are some other interesting findings in this study. The team found significant differences in many biological measurements between men and women with chronic fatigue syndrome. This surely will lead to larger studies to verify these gender-based differences, and to determine what causes them.
There was no difference between people with CFS and the healthy comparison group in the frequency of psychiatric disorders — currently, or in the past. That is, the symptoms of the illness could not be attributed to psychological causes.
Is chronic fatigue syndrome all in the brain?
The NIH team concluded that chronic fatigue syndrome is primarily a disorder of the brain, perhaps brought on by chronic immune activation and changes in the gut microbiome. This is consistent with the results of many previous studies.
The growing recognition of abnormalities involving the brain, chronic activation (and exhaustion) of the immune system, and of alterations in the gut microbiome are transforming our conception of CFS –– at least when caused by a virus. And this could help inform potential treatments.
For example, the NIH team found that some immune system cells are exhausted by their chronic state of activation. Exhausted cells don’t do as good a job at eliminating infections. The NIH team suggests that a class of drugs called immune checkpoint inhibitors may help strengthen the exhausted cells.
What are the limitations of the study?
The number of people who were studied was small: 17 people with ME/CFS and 21 healthy people of the same age and sex, who served as a comparison group. Unfortunately, the study had to be stopped before it had enrolled more people, due to the COVID-19 pandemic.
That means that the study did not have a great deal of statistical power and could have failed to detect some abnormalities. That is the weakness of the study.
The bottom line
This latest study from the NIH joins thousands of previously published scientific studies over the past 40 years. Like previous research, it also finds that people with ME/CFS have measurable abnormalities of the brain, the immune system, energy metabolism, the blood vessels, and bacteria that live in the gut.
What causes all of these different abnormalities? Do they reinforce each other, producing spiraling cycles that lead to chronic illness? How do they lead to the debilitating symptoms of the illness? We don’t yet know. What we do know is that people are suffering and that this illness is afflicting millions of Americans. The only sure way to a cure is studies like this one that identify what is going wrong in the body. Targeting those changes can point the way to effective treatments.
About the Author

Anthony L. Komaroff, MD, Editor in Chief, Harvard Health Letter
Dr. Anthony L. Komaroff is the Steven P. Simcox/Patrick A. Clifford/James H. Higby Professor of Medicine at Harvard Medical School, senior physician at Brigham and Women’s Hospital in Boston, and editor in chief of the Harvard … See Full Bio View all posts by Anthony L. Komaroff, MD

Still confused after Flovent discontinuation? What to know and do

What happens when a widely used medicine is no longer available at pharmacies across the US? Until recently, Flovent (fluticasone) inhalers were frequently prescribed to help control asthma. If you or your child relied on these products, you may be scrambling to find medicines that will help you stay healthy without breaking the bank.
What’s essential to know, and what questions should you ask your health care provider? We checked in with Dr. William B. Feldman, a physician in the Division of Pulmonary and Critical Care Medicine at Harvard-affiliated Brigham and Women’s Hospital to get answers.
Which medicines are discontinued?
In January, GlaxoSmithKline stopped producing Flovent, which was available as a prescription metered-dose inhaler (Flovent HFA) and a dry powder inhaler (Flovent Diskus).
Both contain fluticasone, a steroid. Fluticasone reduces inflammation and swelling in the airways. Both types of inhalers are FDA-approved to help prevent asthma attacks.
However, children under age 5 and adults with particularly poor lung function may not be able to use a dry powder inhaler. They may lack the lung power necessary to breathe in deeply enough to pull the medicine into their airways, Dr. Feldman explains. A metered-dose inhaler could be the best choice for them.
Now that Flovent is discontinued, is a generic product available?
Yes, the drug manufacturer has licensed an authorized generic of both Flovent products: the metered-dose inhaler and the dry powder inhaler.
However, insurance coverage may not pay for the authorized generic because it may cost an insurer more than some other branded medicines. So, you may need to switch to another brand to stay healthy. Call your insurance company to check.
What are your alternatives?
This is a good chance for you and your doctor to review your asthma treatment plan. It may be a good time to make changes.
If you had been using Flovent daily for symptom control, your doctor may recommend:
- Trying an inhaled steroid similar to Flovent. Many types of steroids will work, including beclomethasone (Qvar RediHaler), budesonide (Pulmicort Flexhaler), ciclesonide (Alvesco), and mometasone (Asmanex Twisthaler, Asmanex HFA). “These products use different molecules to do the same job as fluticasone,” says Dr. Feldman.
- Switching to a combination inhaler. New studies suggest this approach may help many people who use Flovent daily for symptom control and only use a short-acting medicine to open airways when an asthma flare occurs (see here and here). If you have intermittent asthma symptoms, talk with your provider about whether you could use a combination inhaler when you start to wheeze or have shortness of breath. This combines a medicine called formoterol with a steroid. Symbicort provides this combination in one inhaler. Although not yet approved by the FDA for this specific use, it is approved in many other countries.
What else do asthma specialists advise people to do?
If your insurance covers the authorized generic, this may be a good choice because you already know how to use the product. But what if insurance won’t cover this?
“Any other inhaled steroid should work for most — but not all — people,” says Dr. Feldman. “There are brand-name metered-dose and dry powder inhalers available, such as those mentioned above.”
Here’s what else to know and do
- Discuss whether it’s safe to switch medicines or type of device. For many people, the answer will be yes. But if your health care provider believes that a metered-dose inhaler is the best choice due to age or poor lung function, ask your insurance company for a formulary exception to cover the authorized generic fluticasone or another metered-dose inhaler. Ask your provider to make the same request.
- If you have a child under 5, you and your doctor should also ask your insurance company for a formulary exception to cover a metered-dose inhaler with a steroid.
- For anyone who needs to switch brands, your new inhaler may look and feel different and may require a new technique when you use it to get the full benefit of the medicine. “When folks switch from one type of inhaler to another, it’s very important to get proper education, ideally from their prescriber. But you can also do this online to understand how to properly use this new product,” says Dr. Feldman.
If you do switch, ask your health care provider to show you how to use the new inhaler in an in-person or virtual visit. If that’s not possible, check your technique by watching these videos created by National Jewish Health, a leading US hospital for respiratory care.
What if you’re not feeling as good on a new asthma medicine?
If you’ve switched and notice worsening symptoms or more asthma attacks, contact your health care provider, Dr. Feldman advises. “They should make sure this isn’t due to improper technique with the new device. It may not be, but it’s important to check and to keep your doctor aware of changes like these.”
Is there a difference between an authorized generic and independent generic medicines?
“With an authorized generic, the brand-name company produces the generic or licenses another company to do that. It’s the exact same medicine as the original brand-name drug. It just doesn’t have the label,” says Dr. Feldman.
Independent generics encourage price competition if several companies make them. “With authorized generics, you don’t see those price decreases to the same extent, because you typically just have one product and it’s totally controlled by the branded company,” he adds.
What if you don’t have insurance, or insurance won’t cover a medicine you need?
“These inhalers have extraordinarily high list prices — $200, $300, $400 per month for the product,” notes Dr. Feldman. Manufacturers negotiate rebates with insurers that may substantially lower the price for an insurance plan.
If you don’t have insurance, you won’t get that lower price. So, it’s worth checking prices for all options: you may find the authorized generic will cost you less than other brand-name inhalers.
About the Author

Francesca Coltrera, Editor, Harvard Health Blog
Francesca Coltrera is editor of the Harvard Health Blog, and a senior content writer and editor for Harvard Health Publishing. She is an award-winning medical writer and co-author of Living Through Breast Cancer and The Breast … See Full Bio View all posts by Francesca Coltrera
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD

Does drinking water before meals really help you lose weight?

If you’ve ever tried to lose excess weight, you’ve probably gotten this advice: drink more water. Or perhaps it was more specific: drink a full glass of water before each meal.
The second suggestion seems like a reasonable idea, right? If you fill your stomach with water before eating, you’ll feel fuller and stop eating sooner. But did that work for you? Would drinking more water throughout the day work? Why do people say drinking water can help with weight loss — and what does the evidence show?
Stretching nerves, burning calories, and thirst versus hunger
Three top theories are:
Feel full, eat less. As noted, filling up on water before meals has intuitive appeal. Your stomach has nerves that sense stretch and send signals to the brain that it’s time to stop eating. Presumably, drinking before a meal could send similar signals.
- The evidence: Some small, short-term studies support this idea. For example, older study subjects who drank a full glass of water before meals tended to eat less than those who didn’t. Another study found that people following a low-calorie diet who drank extra water before meals had less appetite and more weight loss over 12 weeks than those on a similar diet without the extra water. But neither study assessed the impact of drinking extra water on long-term weight loss.
Burning off calories. The water we drink must be heated up to body temperature, a process requiring the body to expend energy. The energy spent on this — called thermogenesis — could offset calories from meals.
- The evidence: Though older studies provided some support for this explanation, more recent studies found no evidence that drinking water burned off many calories. That calls the thermogenesis explanation for water-induced weight loss into question.
You’re not hungry, you’re thirsty. This explanation suggests that sometimes we head to the kitchen for something to eat when we’re actually thirsty rather than hungry. If that’s the case, drinking calorie-free water can save us from consuming unnecessary calories — and that could promote weight loss.
- The evidence: The regulation of thirst and hunger is complex and varies over a person’s lifespan. For example, thirst may be dulled in older adults. But I could find no convincing studies in humans supporting the notion that people who are thirsty misinterpret the sensation for hunger, or that this is why drinking water might help with weight loss.
Exercise booster, no-cal substitution, and burning fat demands water
Being well-hydrated improves exercise capacity and thus weight loss. Muscle fatigue, cramping, and heat exhaustion can all be brought on by dehydration. That’s why extra hydration before exercise may be recommended, especially for elite athletes exercising in warm environments.
- The evidence: For most people, hydrating before exercises seems unnecessary, and I could find no studies specifically examining the role of hydration to exercise-related weight loss.
Swapping out high calorie drinks with water. Yes, if you usually drink high-calorie beverages (such as sweetened sodas, fruit juice, or alcohol), consistently replacing them with water can aid weight loss over time.
- The evidence: A dramatic reduction in calorie intake by substituting water for higher-calorie beverages could certainly lead to long-term weight loss. While it’s hard to design a study to prove this, indirect evidence suggests a link between substituting water for high-cal beverages and weight loss. Even so, just as calorie-restricting diets are hard to stick with over the long term, following a water-only plan may be easier said than done.
Burning fat requires water. Dehydration impairs the body’s ability to break down fat for fuel. So, perhaps drinking more water will encourage fat breakdown and, eventually, weight loss.
- The evidence: Though some animal studies support the idea, I could find no compelling evidence from human studies that drinking extra water helps burn fat as a means to lose excess weight.
The bottom line
So, should you bump up hydration by drinking water before or during meals, or even at other times during the day?
Some evidence does suggest this might aid weight loss, at least for some people. But those studies are mostly small or short-term, or based on animal data. Even positive studies only found modest benefits.
That said, if you think it’s working for you, there’s little downside to drinking a bit more water, other than the challenge of trying to drink if you aren’t particularly thirsty. My take? Though plenty of people recommend this approach, it seems based on a theory that doesn’t hold water.
About the Author

Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing; Editorial Advisory Board Member, Harvard Health Publishing
Dr. Robert H. Shmerling is the former clinical chief of the division of rheumatology at Beth Israel Deaconess Medical Center (BIDMC), and is a current member of the corresponding faculty in medicine at Harvard Medical School. … See Full Bio View all posts by Robert H. Shmerling, MD

Ever worry about your gambling?

Are online gambling and sports betting new to your area? Are gambling advertisements catching your eye? Have you noticed sports and news shows covering the spread? Recent changes in laws have made gambling widely accessible, and its popularity has soared.
Occasional bets are rarely an issue. But uncontrolled gambling can lead to financial, psychological, physical, and social consequences, some of which are extreme. Understanding whether gambling is becoming a problem in your life can help you head off the worst of these issues and refocus on having more meaning, happiness, and psychological richness in your life. Gambling screening is a good first step.
Can you screen yourself for problem gambling?
Yes. Screening yourself is easy. The Brief Biosocial Gambling Screen (note: automatic download) is a validated way to screen for gambling disorder. It has three yes-or-no questions. Ask yourself:
- During the past 12 months, have you become restless, irritable, or anxious when trying to stop/cut down on gambling?
- During the past 12 months, have you tried to keep your family or friends from knowing how much you gambled?
- During the past 12 months, did you have such financial trouble as a result of your gambling that you had to get help with living expenses from family, friends, or welfare?
What do your answers mean?
Answering yes to any one of these questions suggests that you are at higher risk for experiencing gambling disorder. Put simply, this is an addiction to gambling. Like other expressions of addiction, for gambling this includes loss of control, craving, and continuing despite bad consequences. Unique to gambling, it also often means chasing your losses.
A yes doesn’t mean that you are definitely experiencing a problem with gambling. But it might be valuable for you to seek a more in-depth assessment of your gambling behavior. To find an organization or person qualified to help, ask a health care provider, your local department of public health, or an advocacy group like the National Council on Problem Gambling.
Are you ready for change?
Your readiness to change a behavior matters when deciding the best first steps for making a change. If someone asks you whether you want to change your gambling, what would you say?
|
I never think about my gambling. |
Sometimes I think about gambling less. |
I have decided to gamble less. |
I am already trying to cut back on my gambling. |
I changed my gambling: I now do not gamble, or gamble less than before. |
Depending on your answer, you might seek out different solutions. What’s most important initially is choosing a solution that feels like the right fit for you.
What if you don’t feel ready to change? If you haven’t thought about your gambling or only occasionally think about changing your gambling, you might explore lower intensity actions. For example, you could
- read more about how gambling could create a problem for you
- listen to stories of those who have lived experience with gambling disorder.
If you are committed to making a change or are already trying to change, you might seek out more engaging resources and strategies to support those decisions, like attending self-help groups or participating in treatment.
Read on for more details on choices you might make.
What options for change are available if you want to continue gambling?
If you want to keep gambling in some way, you might want to stick to lower-risk gambling guidelines:
- gamble no more than 1% of household income
- gamble no more than four days per month
- avoid regularly gambling at more than two types of games, such as playing the lottery and betting on sports.
Other ways to reduce your risk of gambling harm include:
- Plan ahead and set your own personal limits.
- Keep your entertainment budget in mind if you decide to gamble.
- Consider leaving credit cards and debit cards at home and use cash instead.
- Schedule other activities directly after your gambling to create a time limit.
- Limit your use of alcohol and other drugs if you decide to gamble.
What are easy first steps toward reducing or stopping gambling?
If you’re just starting to think about change, consider learning more about gambling, problem gambling, and ways to change from
- blogs, like The BASIS
- books like Change Your Gambling, Change Your Life
- podcasts like After Gambling, All-In, and Fall In, which offer expert interviews, personal recovery stories, and more.
Some YouTube clips demystify gambling, such as how slot machines work, the limits of skill and knowledge in gambling, and how gambling can become an addiction. These sources might help you think about your own gambling in new ways, potentially identifying behaviors that you need to change.
What are some slightly more active steps toward change?
If you’re looking for a slightly more active approach, you can consider engaging in traditional self-help experiences such as helplines and chatlines or Gamblers Anonymous.
Another option is self-help workbooks. Your First Step to Change is a popular workbook that provides information about problem gambling, self-screening exercises for gambling and related conditions like anxiety and depression, and change exercises to get started. A clinical trial of this resource suggested that users were more likely than others to report having recently abstained from gambling.
Watch out for gambling misinformation
As you investigate options, keep in mind that the quality of information available can vary and may even include misinformation. Misinformation is incorrect or misleading information. Research suggests that some common types of gambling misinformation might reinforce harmful beliefs or risky behaviors.
For example, some gambling books, websites, and other resources exaggerate your likelihood of winning, highlight win and loss streaks as important (especially for chance-based games like slots), and suggest ways to change your luck to gain an edge. These misleading ideas can help you to believe you’re more likely to win than you actually are, and set you up for failure.
The bottom line
Taking a simple self-screening test can start you on a journey toward better gambling-related health. Keep in mind that change can take time and won’t necessarily be a straight path.
If you take a step toward change and then a step back, nothing is stopping you from taking a step forward again. Talking with a care provider and getting a comprehensive assessment can help you understand whether formal treatment for gambling is a promising option for you.
About the Author

Debi LaPlante, PhD, Contributor
Dr. Debi LaPlante is director of the division on addiction at the Cambridge Health Alliance, and an associate professor of psychiatry at Harvard Medical School. She joined the division in 2001 and is involved with its … See Full Bio View all posts by Debi LaPlante, PhD

Stepping up activity if winter slowed you down

If you've been cocooning due to winter’s cold, who can blame you? But a lack of activity isn't good for body or mind during any season. And whether you're deep in the grip of winter or fortunate to be basking in signs of spring, today is a good day to start exercising. If you’re not sure where to start — or why you should — we’ve shared tips and answers below.
Moving more: What’s in it for all of us?
We’re all supposed to strengthen our muscles at least twice a week and get a total at least 150 minutes of weekly aerobic activity (the kind that gets your heart and lungs working). But fewer than 18% of U.S. adults meet those weekly recommendations, according to the CDC.
How can choosing to become more active help? A brighter mood is one benefit: physical activity helps ease depression and anxiety, for example. And being sufficiently active — whether in short or longer chunks of time — also lowers your risk for health problems like
- heart disease
- stroke
- diabetes
- cancer
- brain shrinkage
- muscle loss
- weight gain
- poor posture
- poor balance
- back pain
- and even premature death.
What are your exercise obstacles?
Even when we understand these benefits, a range of obstacles may keep us on the couch.
Don’t like the cold? Have trouble standing, walking, or moving around easily? Just don’t like exercise? Don’t let obstacles like these stop you anymore. Try some workarounds.
- If it’s cold outside: It’s generally safe to exercise when the mercury is above 32° F and the ground is dry. The right gear for cold doesn’t need to be fancy. A warm jacket, a hat, gloves, heavy socks, and nonslip shoes are a great start. Layers of athletic clothing that wick away moisture while keeping you warm can help, too. Consider going for a brisk walk or hike, taking part in an orienteering event, or working out with battle ropes ($25 and up) that you attach to a tree.
- If you have mobility issues: Most workouts can be modified. For example, it might be easier to do an aerobics or weights workout in a pool, where buoyancy makes it easier to move and there’s little fear of falling. Or try a seated workout at home, such as chair yoga, tai chi, Pilates, or strength training. You’ll find an endless array of free seated workout videos on YouTube, but look for those created by a reliable source such as Silver Sneakers, or a physical therapist, certified personal trainer, or certified exercise instructor. Another option is an adaptive sports program in your community, such as adaptive basketball.
- If you can’t stand formal exercise: Skip a structured workout and just be more active throughout the day. Do some vigorous housework (like scrubbing a bathtub or vacuuming) or yard work, climb stairs, jog to the mailbox, jog from the parking lot to the grocery store, or do any activity that gets your heart and lungs working. Track your activity minutes with a smartphone (most devices come with built-in fitness apps) or wearable fitness tracker ($20 and up).
- If you’re stuck indoors: The pandemic showed us there are lots of indoor exercise options. If you’re looking for free options, do a body-weight workout, with exercises like planks and squats; follow a free exercise video online; practice yoga or tai chi; turn on music and dance; stretch; or do a resistance band workout. Or if it’s in the budget, get a treadmill, take an online exercise class, or work online with a personal trainer. The American Council on Exercise has a tool on its website to locate certified trainers in your area.
Is it hard to find time to exercise?
The good news is that any amount of physical activity is great for health. For example, a 2022 study found that racking up 15 to 20 minutes of weekly vigorous exercise (less than three minutes per day) was tied to lower risks of heart disease, cancer, and early death.
"We don't quite understand how it works, but we do know the body's metabolic machinery that imparts health benefits can be turned on by short bouts of movement spread across days or weeks," says Dr. Aaron Baggish, founder of Harvard-affiliated Massachusetts General Hospital's Cardiovascular Performance Program and an associate professor of medicine at Harvard Medical School.
And the more you exercise, Dr. Baggish says, the more benefits you accrue, such as better mood, better balance, and reduced risks of diabetes, high blood pressure, high cholesterol, and cognitive decline.
What’s the next step to take?
For most people, increasing activity is doable. If you have a heart condition, poor balance, muscle weakness, or you’re easily winded, talk to your doctor or get an evaluation from a physical therapist.
And no matter which activity you select, ease into it. When you’ve been inactive for a while, your muscles are vulnerable to injury if you do too much too soon.
“Your muscles may be sore initially if they are being asked to do more,” says Dr. Sarah Eby, a sports medicine specialist at Harvard-affiliated Spaulding Rehabilitation Hospital. “That’s normal. Just be sure to start low, and slowly increase your duration and intensity over time. Pick activities you enjoy and set small, measurable, and attainable goals, even if it’s as simple as walking five minutes every day this week.”
Remember: the aim is simply exercising more than you have been. And the more you move, the better.
About the Author

Heidi Godman, Executive Editor, Harvard Health Letter
Heidi Godman is the executive editor of the Harvard Health Letter. Before coming to the Health Letter, she was an award-winning television news anchor and medical reporter for 25 years. Heidi was named a journalism fellow … See Full Bio View all posts by Heidi Godman
About the Reviewer

Howard E. LeWine, MD, Chief Medical Editor, Harvard Health Publishing
Dr. Howard LeWine is a practicing internist at Brigham and Women’s Hospital in Boston, Chief Medical Editor at Harvard Health Publishing, and editor in chief of Harvard Men’s Health Watch. See Full Bio View all posts by Howard E. LeWine, MD